Why has “Integrated Healthcare” existed as a buzzword in the United States? In many ways, it is because staff and the people they serve have yet to see the entire concept come to life. Implementations have failed. Expected outcomes are unclear. Business models are not fully thought through. Healthcare professionals are still in a learning phase. The public wades through it along with the other confusing healthcare terms they hear in the news. So how do we move away from this phase and move toward providing the care that so many millions need?
Like most things, getting started is the hardest part.
The best place to start is by establishing a clear and shared vision for your organization’s entry into Integrated Healthcare. It is a journey that will bring on many decision points, and it won’t always be obvious which is right for you. Having an agreed upon vision is essential to most projects, but even more so for Integrated Healthcare. It is brand new territory for most teams and the landscape can vary dramatically from one organization to the next.
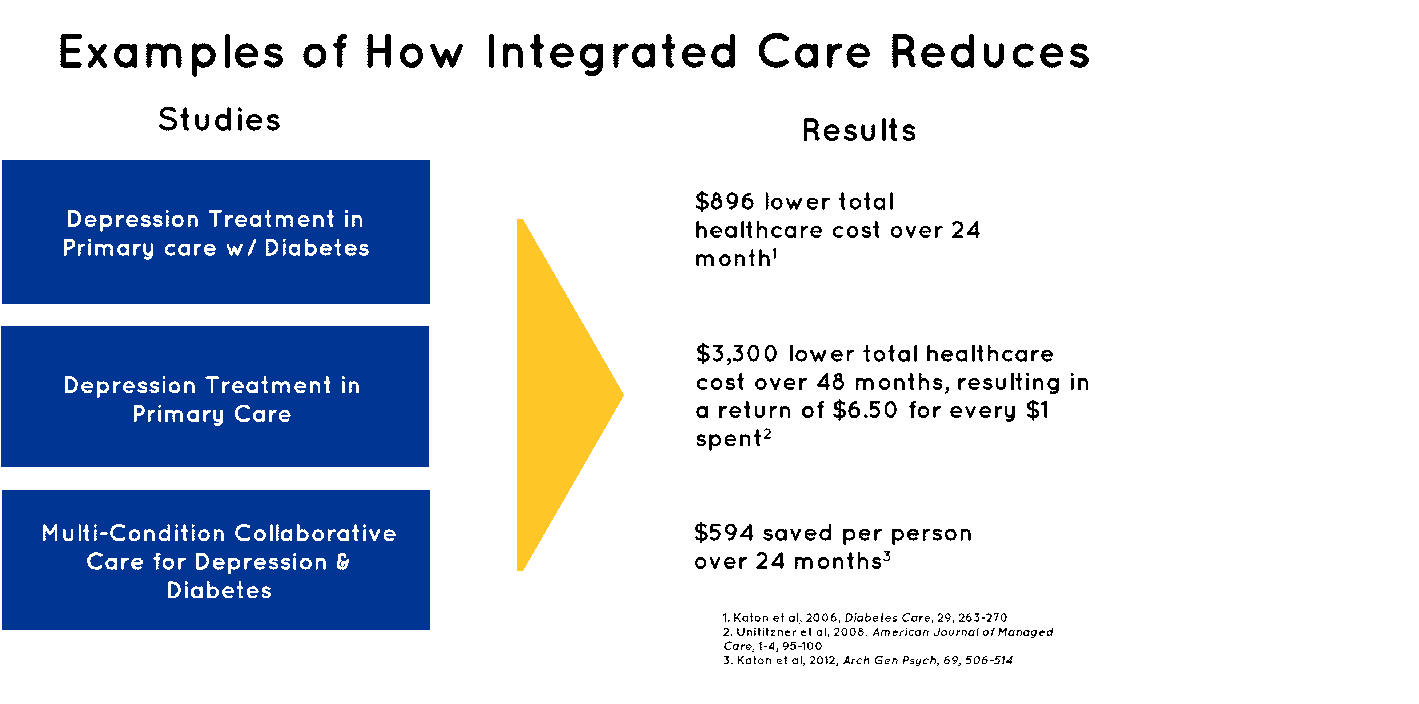
Having documented research on hand, like the facts below, can help drive the conversation and get things moving when trying to round out your specific mission and achieve buy-in:
Once you’ve established your vision, assessing the readiness of your organization is the next step. SAMHSA’s Readiness Assessment is widely accepted as a standard in the industry. It is a wonderful tool, but can be difficult to self-administer because of the details and complexities of the concepts that it is trying to evaluate.
This assessment will give you your baseline and help you to easily identify your short and long term goals throughout the process. Beyond the baseline, it also provides a clear picture of what your organization will need to work on to create a successful program. This will help to identify the scope of work necessary to implement your model, so in cases where there are limited resources this process will help prevent you from beginning a project your organization is not ready to execute.
As is often the case in healthcare, the lack of a common language or definitions can hold us back. From one conversation to the next, you can sense the confusion around integrated care, because it can mean so many different things to different people.
It is critical to develop a common language across the industry, but more importantly, among your staff. What model of integrated care are you going to implement? What do you call it? Why did you choose it? These questions are often glossed over or ignored altogether during the process – leading to confusion or misunderstanding from your teams about your Integrated Health initiatives.
The key is to keep collaboration high among the staff involved. Discuss how you will address questions together. Make it easy for everyone to understand and explain the concepts. Developing a common language can be a difficult task to focus on, but you will be grateful you did. Don’t let it get lost in the list of other tasks. Make sure it is a priority item for your team, because in the long run this will help to create alignment and better understanding around your programs and their purpose.
So now that you know why your organization is entering into the world of Integrated Health, and you’ve identified your baseline – now what?
Choosing which model is right for your business and community is where the process moves from learning to action. There are a variety of models that can work for any given organization, but it is is a decision that you should make very deliberately.
Important questions to ask
This is a lot to sort through and it can be difficult for organizations to define their model when they don’t have experience with these concepts across the physical health, behavioral health, and social service components needed for a strong Integrated Health business model. Having support throughout this process from subject matter experts in each area is imperative, because this will help to bridge the needs, issues, and language to ensure a program that will positively affect your patient population.
Once you’ve chosen your model, the real work begins. The project team is typically already assembled by this point, but if not make sure you formalize who the people will be that are primarily responsible for this significant change effort. You don’t want the hard work you’ve put in to the preparation lost in the detail of the daily implementation tasks.
Tips on how to ensure you develop a proper plan
Way back when you set your vision and went through the assessment process you established some areas where you wanted to measure success. During many large projects, it is easy to lose site of the end game. Throughout your process, make sure that you are focusing on the data points that are critical to your mission as well as those that are important to your partners.
From state specific requirements to critical clinical measurements, you need to have a plan for collecting and extracting data in a meaningful way. This data will allow to sustain your model and position your organization to make the case for integration and expanded partnerships.
Sound like a lot of work? It is, but it is truly worth the effort.
People with mental illness die 25 years earlier than the general population due to preventable conditions.
At Afia, we’re committed to making sure that number is history. We have a passionate, experienced team that has seen how this can change the lives of those you serve. We know how to make sure you create a sustainable business model as well. We know how to turn well-intentioned words into action and visions into reality.
If we can help in any way, please let us know. We’re here to help.
All Thought Leadership